Burns: Nutrition
![]()
Your child is being treated for a burn and needs good nutrition to help him or her heal. Your child’s body uses a lot of extra energy as it works to heal the skin. His daily nutrition is very important. How much and what kind of nutrition your child needs will depend on the type and severity of the burn wounds. The dietitian will carefully assess your child’s individual needs for protein, carbohydrates, fats, vitamins, and minerals.The dietitian and nurses will teach you how to help your child meet these nutrition goals. They will check your child’s progress on a daily basis. Good nutrition is still important to help heal burns and other wounds, even months after the injury.
What to Eat
We recommend and encourage high calorie, high protein foods for burn patients. Examples of high protein foods (see Picture 1) are:
- Dairy products (milk, cheese, milkshakes, ice cream)
- Meats and fish
- Eggs
- Nuts and nut or seed butters (almond, peanut, walnut, pecan, cashew, sesame, sunflower, etc.)
- Beans and legumes (kidney, white, garbanzo, navy, black, soy and pinto beans; lentils, peas, hummus, etc.)
- Formulated drinks (such as Ensure® and Pediasure®)
Benefits of Good Nutrition
While your child is healing, it is especially important for him to get good nutrition. Your child’s body needs extra energy while trying to heal. Eating enough healthy foods will help to:
- Promote healing
- Fight and prevent infection
- Support the higher demands on your child’s body
Recording Food and Drink
Your child will need to keep a daily record of what he or she eats and drinks. Food and liquids taken in by mouth (oral intake) will be recorded on a paper labeled ‘Calorie Counts’ that will be placed on the door to your child’s room each day. This helps dietitians, doctors, and nurses keep track of your child’s progress in meeting his or her nutritional needs.
Recording Weight
Your child will be weighed every day, or as ordered by the doctor.
Recording Output
Recording how much your child goes to the bathroom helps the medical team know if he or she is eating and drinking enough. If your child is in diapers, do not throw the diapers away when you change them. It is important to keep the used diapers in the bathroom for staff to weigh them. If your child is potty trained, there will be a measuring device in the toilet for urine. Boys can use a urinal. It is important that the staff knows how much urine your child is making to be sure he or she is getting enough liquids.
Tube Feeds
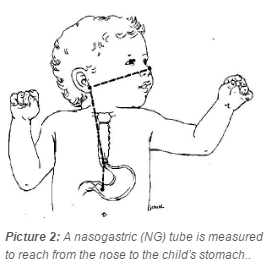
If your child is not able to take in enough nutrition by mouth, he or she will likely need to be fed through a tube. If tube feeding is needed, a nasogastric tube (NG tube) is inserted into the nose and slid into the stomach (see Picture 2). A formula recommended by the dietitian and doctor will be given through the NG tube.
The goal is for your child to take in the amount of nutrition needed to help the burns to heal. How long a child needs to stay on formula is based on the child’s ability to start eating and drinking enough by mouth. If your child cannot get enough nutrition from food and drink alone, the tube feed will likely need to run all the time.
When your child can take in more by mouth, tube feeds will eventually be given for shorter periods of time, until they are no longer needed.
PICC Line
Depending on your child’s condition, the medical team may have a PICC (Peripherally Inserted Central Catheter) put in. A PICC is a plastic tube that is inserted into a large vein to give intravenous (IV) therapy (nutrition or medicine). Through the PICC line, liquid nutrition called TPN (Total Parenteral Nutrition) will be given. TPN is a way to provide all the nutrients and calories needed when a person cannot eat, or cannot eat enough.
When to Call the Doctor
After your child is discharged from the hospital, please call the clinic at (614) 722-3900 if:
- Your child has lost weight.
- Your child is eating or drinking less.
- Burns are not healing.
- There are signs of infection (unusual drainage, a bad smell, or fever greater than 101 degrees Fahrenheit taken under the tongue).
- You have any nutritional or diet questions or concerns.
HH-IV-152 4/15 Copyright 2015, Nationwide Children’s Hospital
