Birth Control: Hormonal Intrauterine Device (IUD)

The hormonal intrauterine device (IUD) (Picture 1) is a small, T-shaped plastic device with strings attached. The hormonal IUD contains a small amount of progestin similar to the hormone your body makes naturally. The hormonal IUD works mainly by thickening the cervical mucus to keep the sperm from joining with an egg.
Advantages of the Hormonal IUD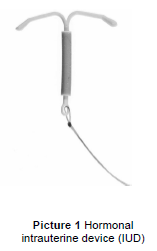
- more than 99% effective
- lasts up to 3 to 8 years depending on the type
- some types may be used as emergency contraception
- completely reversible once removed
- fewer menstrual cramps
- lighter periods
- safe with breastfeeding
- can be put in immediately after giving birth
- some users stop having periods completely
Disadvantages of the Hormonal IUD
- Spotting and irregular vaginal bleeding between periods for the first several months after it is put in is common.
- Cramping and some discomfort can occur at the time it is put in.
How it is Put In
The hormonal IUD is put into your uterus by a health care provider after a pelvic exam. The IUD is inserted through the opening in your cervix into the uterus. You may feel cramping while it is being put in. Speak with your health care provider about what to do if you have pain.
How it is Taken Out
Your IUD may be removed at a simple office visit. Your health care provider will put a speculum (the same instrument used for a pelvic exam) inside the vagina to make it easier to see the strings of the IUD. Then, they will gently pull the strings to take it out. Having the IUD taken out takes less time and is usually less uncomfortable than having it put in. If the IUD strings cannot be seen, or the IUD cannot be taken out this way, you may need an extra procedure.
Risks
- Perforation: It is rare, but an IUD can be pushed into or through the wall of the uterus while it is being put in. This is called perforation. Sometimes surgery is needed to remove the IUD.
- Expulsion: Sometimes the IUD can partly or completely slip out of the uterus. This is called expulsion. You can become pregnant if it happens.
- Pregnancy: The risk of pregnancy with an IUD is very small. If it does happen, there is a higher risk of tubal pregnancy, infection, miscarriage and early labor and delivery. These problems can be life-threatening. The IUD should be taken out if this happens.
- Infection: It is very rare, but the IUD can be linked to pelvic inflammatory disease (PID). Most PID happens within three weeks of insertion. It is linked to sexually transmitted infections (STIs) like chlamydia or gonorrhea.
Who Cannot Use Them
The hormonal IUD should not be used by those who:
- have or think they may have an STI or a pelvic infection
- have had a pelvic infection in the last three months
- have certain abnormalities of the uterus
- have unexplained vaginal bleeding that has not been discussed with their provider
Tell your health care provider if you have any of these risk factors or conditions, or any other medical concerns.
When to Call the Health Care Provider
Call the doctor or health care provider right away if you:
- think you are pregnant
- think you might have an STI
- have unusual vaginal discharge
- have unexplained fever or chills
- have pain or bleeding with sex
- have unusual or very heavy bleeding from the vagina
- notice any change in the length of the string or can feel part of the IUD
- have unusual pelvic pain, cramping, or soreness in your abdomen (belly)
Preventing STIs
The hormonal IUD does not protect against sexually transmitted infections (STIs). Condoms are the best way for sexually active people to reduce the risk of infection. Always use a condom when you have sex. Get yearly health check-ups, including testing for STIs
HH-IV-26 ©1977, Revised 9/2022, Nationwide Children’s Hospital

