Cardiopulmonary Resuscitation (CPR): Age 1 to Puberty

Cardiopulmonary resuscitation (kar-dee-oh-pul-muh-nayr-ee ree-suh-sih-tay-shun), also called CPR, is a way you can save someone’s life if they stop breathing or their heart stops. It combines chest pumping (compressions), which moves blood from the heart to the body, and mouth-to-mouth breathing, which sends oxygen to the lungs.
How the Lungs and Heart Work
The lungs’ purpose is to breathe in (inhale) air that is made of oxygen, which we need to live. The heart pumps the blood to the lungs and the body. The heart and the lungs work together to send oxygen in the blood to the rest of the body.If the Child Stops Breathing or the Heart Stops Beating
If your child stops breathing, they're not getting the oxygen they need to stay alive. If breathing stops, the heart will also stop soon.
YOU MUST ACT RIGHT AWAY BY:
- Pumping the child's heart with your hand (compressing).
- Breathing air into the child’s lungs (ventilating).
Practice
- IMPORTANT: You must practice CPR on a doll (mannequin) with a nurse to be sure you’re doing it correctly. This should be done before you leave the hospital with your child.
- If you wish to become certified in CPR, contact the American Heart Association® or the Red Cross® in your community.
How to Do CPR
If you think the child is not breathing:
- Check to see if they will respond to you. Tap them gently and shake their shoulders to see if they will move.
- Call them by name and ask, “Are you okay?”
- If they do not respond, call out for someone to call 911 or use your cell phone to call 911 and put it on speakerphone while you start CPR.
- Place them on the floor. CPR must be performed on a hard surface to work.
- Turn them on their back.
- Look at their face and chest to see if they’re breathing. Look for at least 5 seconds but no more than 10 seconds.
- Remove clothing from their chest.
- Place the heel of your hand on the lower half of the breastbone between the nipples. Using one hand, push (compress) their chest 30 times by pressing the breastbone in about 2 inches (see "Quick Reference for CPR" below, step 2). If you aren’t able to push down about 2 inches with one hand, use two hands. Compress the chest fast at a rate of 100 to 120 each minute. It will feel like you’re pushing hard. Let the chest come back to its normal position after each compression.
- After you have compressed the chest 30 times, open their airway for mouth-to-mouth breathing, using the head tilt-chin lift method (see "Quick Reference for CPR" below, step 3). Tip the head back with one hand on the forehead. Use the tips of the fingers of your other hand to lift the chin upward. Be careful not to close their mouth all the way.
- Give them 2 breaths (see "Quick Reference for CPR" below, step 4). To do this, pinch their nose and cover their mouth with your mouth to form an airtight seal. Breathe into their mouth only enough air to make the chest rise. Remove your mouth after each breath and let the air come out. Since a child’s lungs are small, they need less air to fill than an adult’s lungs.
- Repeat 30 compressions and 2 breaths until help arrives.
- If you still have not called 911 because you’re alone and do not have a cell phone, call 911 after 5 sets of 30 compressions and breaths. Keep doing CPR until help arrives. If help is already on the way and the child is not moving or breathing, continue CPR.
Resources: 2015 AHA Guidelines : Update for CPR and ECC
Quick Reference for CPR
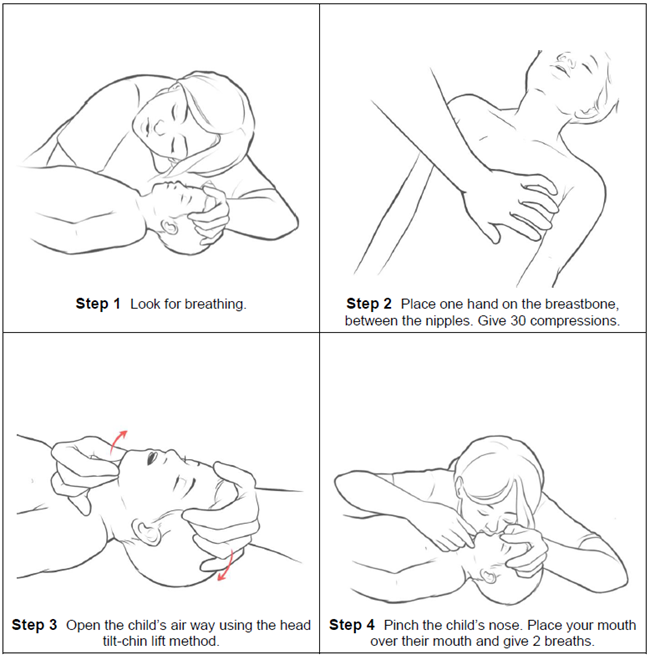
HH-II-47 • ©1983, revised 2023 • Nationwide Children's Hospital
