PIVOTAL Network
The PIVOTAL Network is a group of healthcare providers, institutions, and researchers working in collaboration to determine the best approach to treat preterm infants diagnosed with patent ductus arteriosus, commonly referred to as a PDA.
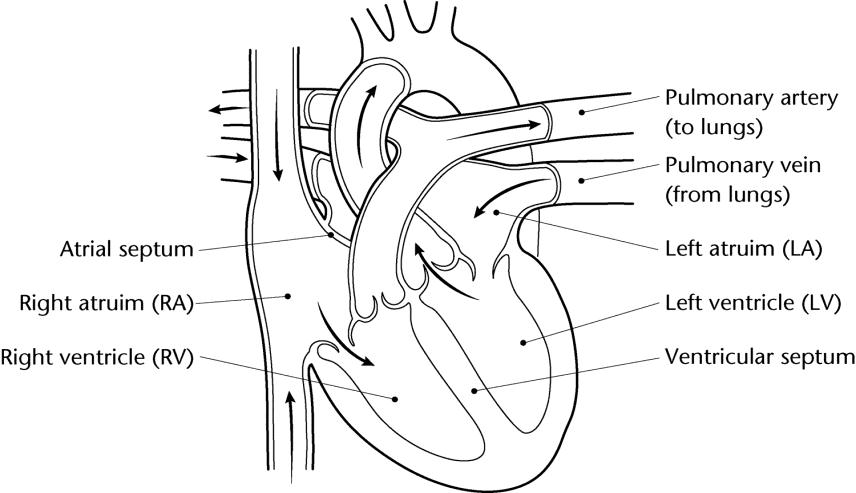
Above: Inside a healthy heart
What is a Patent Ductus Arteriosus?
- The ductus arteriosus is a blood vessel present in all unborn infants, allowing blood to bypass the lungs while in the womb.
- The ductus normally closes within a couple of days after birth, after the baby begins to breathe on it’s own.
- When it does not, it is called a patent ductus arteriosus, and is a congenital heart defect
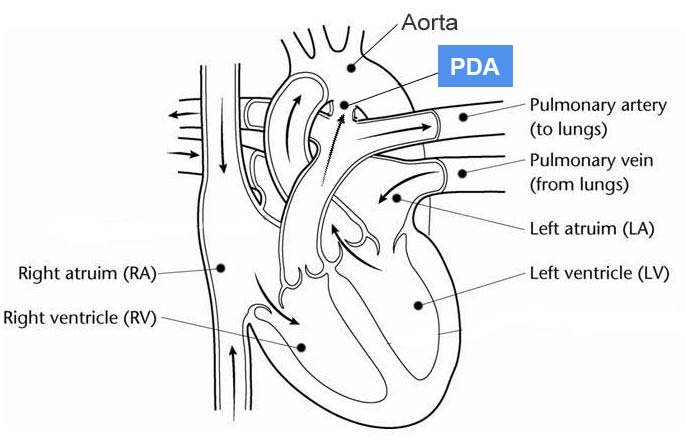
Above: Inside a heart with patent ductus arteriosus.
PDA and Prematurity
- Premature infants are more likely to have a PDA than infants born at term.
- Younger gestational age increases the likelihood of PDA in premature infants.
- Natural closure of PDA in premature infants may occur, but this may take much longer than normal.
Risks of PDA in Preterm Infants
A PDA may cause serious problems, especially for preterm infants:
- Difficulty breathing normally
- Difficulty eating and gaining weight
- Development of pulmonary hypertension
- Changes in size, shape, and function of the heart
Treatment of PDA in Preterm Infants
Additional Resources
- In order to allow time for natural closure, doctors may recommend a “wait and see” approach. This is called conservative management.
- Doctors may recommend procedures to close PDA in premature infants:
- Medications to promote closure
- Catheter-based closure
- Surgical ligation
Pharmaceutical (Drug) Closure of PDA
Pharmaceutical (Drug) Closure of PDA
- Premature infants may be given medications to promote closure of the PDA:
- Indomethacin
- Ibuprofen
- Acetaminophen
- Medications may be tried before any other treatment is recommended
Advantages
- Successful in ??% of cases
Risks
- Lower gestational age decreases chances of success
- Reduced blood flow to intestines (side-effect) may lead to gastrointestinal (gut) complications
Conservative Management of PDA
Conservative Management of PDA
- During conservative management, the doctors may prescribe
- Reduced fluid intake
- Diuretic medications
- Often attempted before more invasive procedures are recommended
Advantages
- No procedural intervention(s)
- High success in higher gestational age premature infants
Risks
- Longer duration of exposure to PDA and diuretic medications
- Restricted weight gain
- May lead to breathing-related complications if prolonged
Catheter-Based Closure of PDA
Catheter-Based Closure of PDA
- This procedure is performed under general anesthesia.
- A small incision is made in the groin, and a wire (catheter) is inserted into a blood vessel and run up to and into the heart.
- Using the catheter, a small device is implanted within the PDA to promote clotting and closure.
Advantages
- Complete occlusion (closure) of PDA within 24 hours in successful cases
- Minimally-invasive procedure
Risks
- Need for blood transfusion due to blood loss during procedure
- Embolization (implant migrates from PDA to downstream blood vessel)
- Anesthesia exposure
Catheter-Based Closure for Premature Infants?
- In January of 2019, the US Food and Drug Administration approved a new device for catheter PDA closure.
- Unlike previous devices, this new occluder was approved for use in preterm infants of 700 grams body weight, or more.
Surgical Ligation of the PDA
Surgical Ligation of the PDA
- Surgical ligation is an invasive surgical procedure.
- An incision is made in the chest, exposing the heart and blood vessels.
- The PDA is either sewn shut, cut (ligated) and sewn, or a clip (similar to a paperclip) is placed.
- Often only done when other procedures cannot be used, or fail to close the PDA.
Advantages
- Definitive closure of PDA
Risks
- Highly invasive procedure
- Infection at surgical site
- Vocal cord paralysis (permanent) due to possible nerve damage
- Post-surgical instability
