How to Help Your Kids Beat the Heat
With summer right around the corner, warmer, more humid conditions are sure to follow. Summer youth sports leagues will be starting soon, making this a good time to review the types of heat-related illness, first-aid, and methods for prevention of these common medical conditions.
It is estimated that 240 persons die each year in the United States of heat-related illness. Heat stroke is ranked third in cause of death of U.S. high school athletes behind head and neck injuries and cardiac conditions. This becomes an even greater concern in younger athletes.
"Youth and adolescent athletes sweat less, create more heat per body mass, and acclimate much slower than adults to warmer environments, putting them at greater risk for heat-related injuries in hot and humid temperatures," states Thomas Pommering, DO, Medical Director for Nationwide Children's Sports Medicine.
How to Recognize Heat-Related Illness
There are several types and degrees of seriousness of heat-related illness. Each can be differentiated by various signs and symptoms:
- Heat Cramps- painful cramping of the muscles of the limbs and abdomen caused by excessive sweating (due to the depletion of salt and water from the body)
- Heat Syncope- weakness, fatigue, and fainting due to loss of salt and water.
- Heat Exhaustion - cool and pale skin, headache, nausea, chills, weakness, unsteadiness, dizziness, rapid pulse, excessive thirst, and muscle cramps.
- Heat Stroke - hot and dry skin, incoherent speech, disorientation, unconsciousness or coma, nausea, seizures, and rapid or irregular pulse. Heat stroke is the failure of the body's heat-control mechanism, which can cause other organ systems to shut down and cause a life-threatening emergency.
What Should Be Done?
The basic first aid for heat cramps, heat syncope, and heat exhaustion is to cool the athlete as quickly as possible. The athlete can be rapidly cooled by moving them to a cool location (shade, air conditioning, etc.), remove sweat saturated clothes (if appropriate), and apply cold towels/water/ice to the athlete's body. Fluid should be replaced by drinking water or IV fluids can be administered by medical professionals. If these conditions go untreated for too long, they can gradually progress to heat stroke.
"Early recognition and intervention are key in avoiding such a situation," says Pommering. The treatment of heat stroke is much the same as that outlined above, except that it must happen as quickly as possible. Emergency Medical Services (911) should be activated immediately and the athlete transported to the nearest hospital for more sophisticated treatment.
How Can This Be Prevented?
The best treatment for any illness is to prevent it from happening altogether and heat-related illnesses are no exception. Encourage kids to listen to their bodies when it comes to thirst and exercise intensity. New research has shown that drinking to thirst is the best way to ensure an athlete maintains appropriate fluid balance in the body during physical activity. Rehydration should also continue between events or practices. Eating a good diet is very important in hot weather, especially when exercising in the heat for a period of days. Athletes should salt their food generously (unless they have an underlying medical condition or family history of high blood pressure) and choose foods that have high sodium content, such as pizza, soup, and pretzels. This is especially true for salty sweaters. This salty diet can be altered back to “normal” once the weather cools down or athletes aren’t exercising for long periods of time on successive days.
Gradually acclimating to the heat over a period of two weeks is extremely important and allows the body to make physiological changes and better tolerate exercise in hot environments. If a child is taking medications, consult your primary care physician to determine if they could increase the risk for heat-related illnesses.
Coaches should avoid practicing during peak temperatures (i.e. 11am to 3pm) on hotter, more humid days. Athletes should wear clothing that is light in weight and color, because darker clothes attract heat. Frequent rest breaks are important in hot, humid weather to allow the body to dissipate heat and will allow the athlete to drink when thirsty. Athletes should be permitted to remove helmets and other equipment during rest breaks. Athletes should be allowed free access to fluids. Lastly, identification of more at-risk athletes (i.e. overweight, out of shape, those who seem to sweat less, have a previous history of a heat illness) may be key in the prevention of heat-related illnesses and should be monitored closely.
Heat-related illnesses are an inherent danger when exercising outdoors in the summer. But always remember: an ounce of prevention is worth a pound of cure! Hopefully the above information will help you and your young athlete take adequate precautions and have a safe, happy, and healthy summer and fall season.
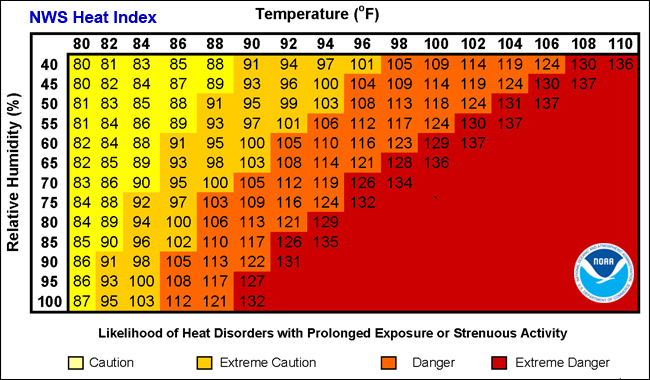
Weather Guide for Activities in Hot, Humid Weather
Below is the National Weather Service Heat Index and recommendations for practice:
- Caution: Water breaks every 15 minutes.
- Extreme Caution: Modify practice intensity. Keep a close eye on kids who are deconditioned and/or have a history of heat illness.
- Danger: Consider changing practice times to a less humid part of the day. Eliminate need for additional equipment/layers. Have a 10 minute rest break every 60 minutes.
- Extreme Danger: Cancel practice.
Consult your primary care physician for more serious injuries that do not respond to basic first aid. As an added resource, the staff at Nationwide Children’s Hospital Sports Medicine is available to diagnose and treat sports-related injuries for youth or adolescent athletes. Services are available in multiple locations. To make an appointment, call (614) 355-6000 or schedule an appointment online.