Rehab Outcomes
Our approach to inpatient rehabilitation focuses on the path ahead. What skills will each patient need to achieve the highest level of independence when he or she returns to home, school and community? We know that every patient’s goal and environment will be different. That’s why we tailor each rehabilitation plan to match the lives of each patient. This model—called outcome-oriented rehabilitation—relies on a partnership between patients, their families, and our highly skilled team of therapists, nurses, physicians and social workers.
Read our Inpatient Rehabilitation Program Annual Report to learn more about what we do and see the outcomes that showcase our efforts.
Demonstrated Differences in Rehab
Focused on Children and Young Adults
Nationwide Children’s Hospital is specialized for the unique needs of children and teens. All of the physician specialists on our Physical Medicine and Rehabilitation team are pediatric trained. Our outcome-oriented rehabilitation plans are designed with physical, cognitive and social development in mind.
Innovative Facilities in a Real-World Setting
Our inpatient unit is outfitted with state-of-the-art equipment that allows patients to work toward recovery in a safe, fun environment. "Determination Way," our custom-designed simulated community, provides a real-world environment where patients learn how to manage activities of daily living.
Continuum of Care
We are located within a leading pediatric medical institution and offer a complete continuum of care all under one roof. Patients have direct access to a range of medical specialties, such as Critical Care, Surgery, Neurology, Neurosurgery, Radiology and Pulmonary Medicine, just to name a few. Access to round-the-clock emergency services means our patients aren’t transferred to another facility when a critical need arises. Our program also accepts patients on ventilators.
Leader in Trauma Care
Nationwide Children’s Hospital is one of the largest American College of Surgeons (ACS) verified Level 1 Pediatric Trauma Centers in the nation. Our Burn Program is nationally recognized as a verified burn program through the American Burn Association.
CARF Accredited for Pediatrics
Our program is recognized by the Commission on Accreditation of Rehabilitation Facilities (CARF) as a Pediatric Specialty Program, an accreditation that recognizes our commitment to providing results-driven, quality services that focus on the unique needs of each patient and family.
Committed to Best Outcomes
Nationwide Children’s is on a journey to create the best outcomes for children everywhere. Through our strategic plan, we will continue to:
- Make every day a safe day for our patients, families and staff
- Help our patients return to their schools and communities
- Expand opportunities for our patients, including those undergoing orthopedic surgery or Selective Dorsal Rhizotomy
- Improve educational opportunities for patients and families
- Facilitate our patients’ independence and increase long-term quality of life outcomes
- Invest in our staff, our programs and our research
2024 Annual Report Highlights

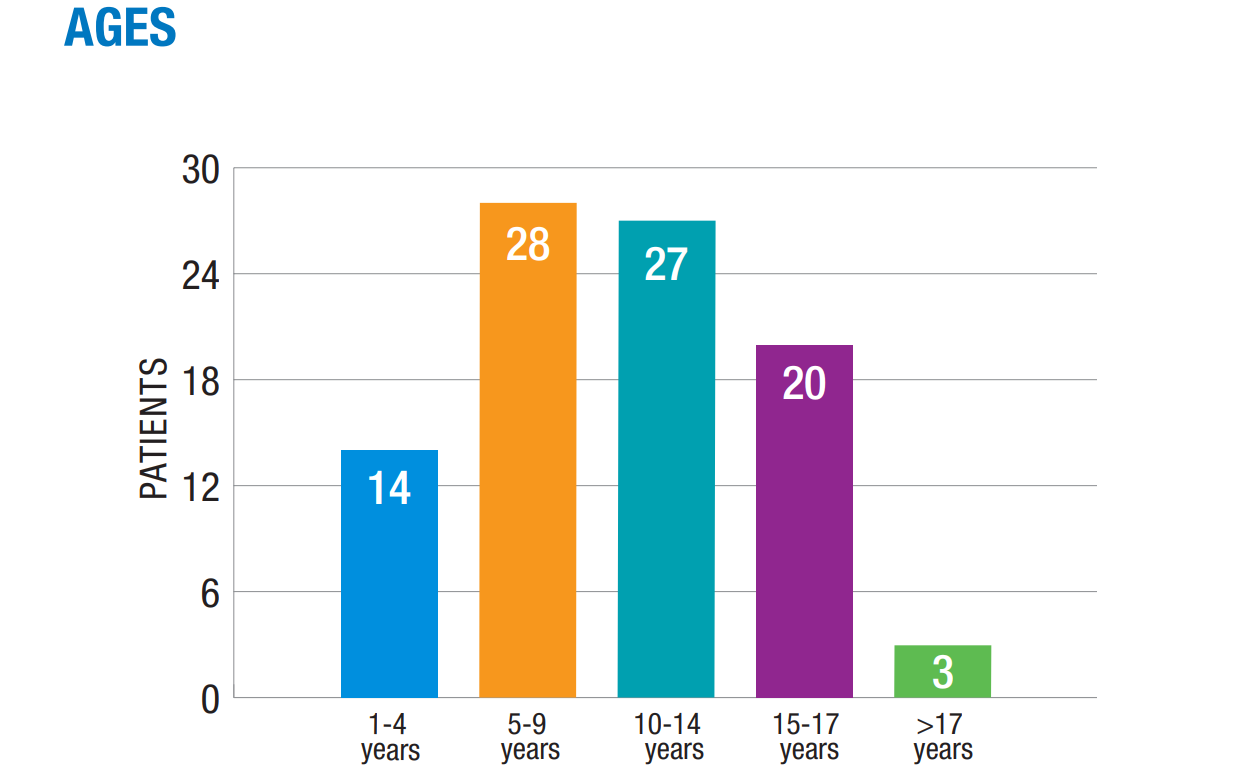





2024 Outcomes: Top Diagnoses
At discharge, 98% (40/41) of our parents, that returned their survey, reported they were Very Satisfied with our program.
Discharges: 25
Age ranges: 2-19 years (average 10 years)
Average length of stay: 21 days
Discharged home: 24/25 = 96%
Unplanned transfers for medical reasons: 2
Average Number of hours of services/day: 4.5
Average functional gain (WeeFIM®): 23 points
Discharges: 15
Age ranges: 2-17 years (average 12.4 years)
Average length of stay: 25 days
Discharged home: 12/15 = 80%
Unplanned transfers for medical reasons: 0
Average Number of hours of services/day: 4.4
Average functional gain (WeeFIM®): 31 points
Discharges: 10
Age ranges: 1-16 years (average 11.4 years)
Average length of stay: 22.3 days
Discharged home: 9/10 = 90%
Unplanned transfers for medical reasons: 0
Average Number of hours of services/day: 4.4
Average functional gain (WeeFIM®): 31 points
Discharges: 17
Age ranges: 4-13 years (average 8 years)
Average length of stay: 14 days
Discharged home: 14/14 = 100%
Unplanned transfers for medical reasons: 0
Average Number of hours of services/day: 4.5
Average functional gain (WeeFIM®): 22 points
Discharges: 13
Age ranges: 2-24 years (average 11 years)
Average length of stay: 28 days
Discharged home: 12/13 = 92%
Unplanned transfers for medical reasons: 1
Average Number of hours of services/day: 4.5
Average functional gain (WeeFIM®): 32 points
Average number of hours of services per day refers to:
- Insurance mandates all Inpatient Rehab Programs to offer 3 hours of OT, PT and or Speech Therapy (or services), 5 days a week.
- Additional services that we include are: Therapeutic Recreation, Child Life, Massage Therapy, Music Therapy, School services and Psychology services, as needed.

