Adolescents with severe obesity who had bariatric surgery showed significant improvements in cardiovascular disease risk factors, according to the most recent “Teen Longitudinal Assessment of Bariatric Surgery” (Teen-LABS) study, published online today by Pediatrics. Prior to bariatric surgery, 33 percent of the study participants had three or more defined cardiovascular disease risk factors. However, three years post-surgery only 5 percent of study participants had three or more risk factors; representing significant reduction in the overall likelihood of developing cardiovascular disease later in life.
Teen-LABS is a multi-center clinical study funded by the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) at the National Institutes of Health (NIH) that is examining the safety and health effects of surgical weight loss procedures in the adolescent population. This on-going study is being conducted at five clinical centers in the U.S., including Cincinnati Children's Hospital, Nationwide Children’s Hospital, Texas Children's Hospital, the University of Alabama at Birmingham, and the University of Pittsburgh Medical Center. The study’s Chair, Thomas H. Inge, MD, PhD, is located at Children’s Hospital Colorado, Denver, CO.
Marc P. Michalsky, MD, surgical director of the Center for Healthy Weight and Nutrition at Nationwide Children's, is the lead author of the latest Teen-LABS publication. The study demonstrated bariatric surgery performed during adolescence may provide unique benefits later in life by altering the probability of the future development of adverse cardiovascular events, including the development and progression of impaired glucose metabolism, atherosclerosis, heart failure and stroke.
"This is the first large-scale analysis of predictors of change in cardiovascular disease risk factors among adolescents following bariatric surgery," said Dr. Michalsky, also a professor of Clinical Surgery and Pediatrics at The Ohio State University College of Medicine. "The study demonstrated early improvement and reduction of cardio-metabolic risk factors, offering compelling support for bariatric surgery in adolescents."
This most recent publication from the Teen-LABS research study extends previous findings describing the baseline prevalence of cardiovascular disease risk factors within the cohort of 242 adolescents. Predictors of change in prevalence of cardiovascular disease risk factors measured included blood pressure, lipids, glucose homeostasis and inflammation.
Three years post-surgery, the study showed a reduction in cardiovascular disease risk factors is associated not only with weight loss, but also with age at the time of surgery, pre-operative body mass index (BMI), sex and race. Specifically, increased weight loss, female sex and younger age at time of surgery serve to predict a higher probability of risk factor resolution. Younger participants were more likely to resolve dyslipidemia compared to older patients, while females were more likely than males to demonstrate improvements in elevated blood pressure.
“Although relationships between change in cardiovascular disease risk factors and postoperative weight reduction were not unexpected, we learned younger patients at time of surgery were more likely to experience dyslipidemia remission and normalization of high sensitivity C-reactive protein (a marker of inflammation), suggesting there may be advantages to undergoing bariatric surgery earlier, even among adolescents,” said Dr. Michalsky. Furthermore, Dr. Michalsky noted that “the results of the current study from Teen-LABS gain further significance when considering newly published data by investigators at Yale University (https://doi.org/10.1016/j.jpeds.2017.09.066) which highlights the long-term impact of significantly elevated cardiovascular disease risk factors observed among a large sample of severely obese youth (Class III and Class IV Obesity) compared to less obese study participants.
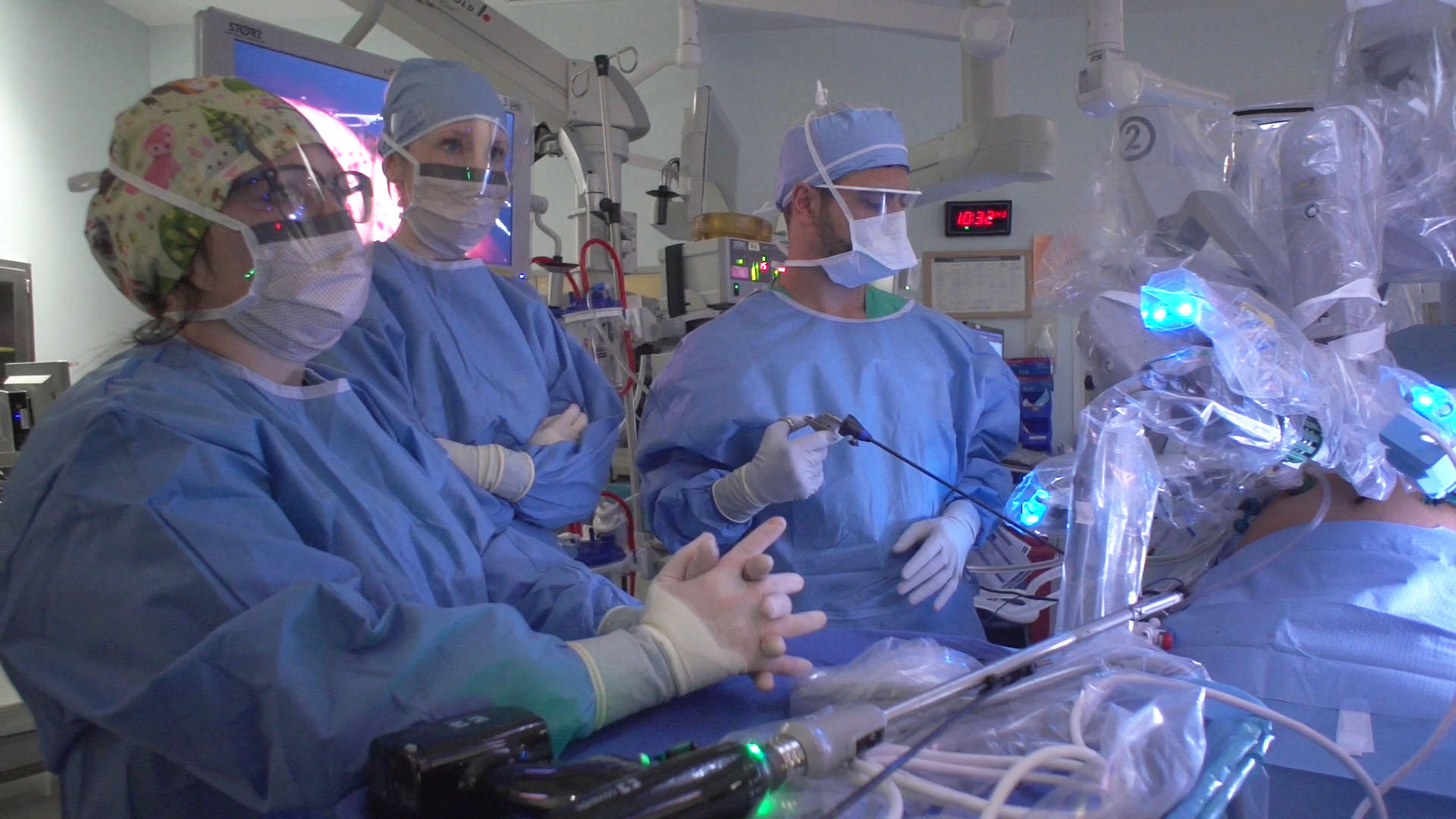
A surgical team at Nationwide Children’s Hospital performs a sleeve gastrectomy on a teenage patient.
Learn more about this study and watch one patient's journey.
Contact the media team to request broadcast quality video and photos.
