Supraventricular Tachycardia (SVT)

The Heart as a Pump
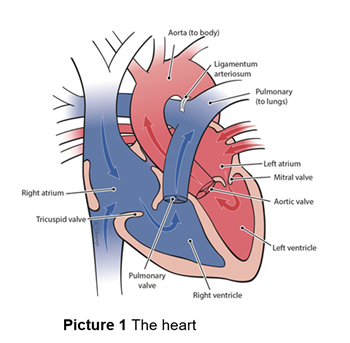
The heart has four chambers. The two on the top are called the atria and the two on the bottom are called the ventricles. The right atrium receives blood from the body and sends it to the right ventricle which pumps the blood to the lungs. The blood returns from the lungs to the left atrium which sends blood to the left ventricle which pumps blood back to the body. For the heart to function as a good pump, the atria must squeeze first, then pause and allow the bottom chambers to pump (Picture 1).
The Heart’s Electrical System
Next, we must understand how the conduction system is built. The normal “pacemaker” of the heart is called the sinus node. It is located at the top of the right atrium. An impulse, or electrical signal, passes from the sinus node through both atria, much like ripples from a pebble thrown into the water. The electrical signal tells the atria to squeeze blood into the ventricles. The signal then travels to the AV node and then down through the electrical pathway. This pathway branches into the right and left ventricles. The electrical impulse stimulates the ventricles to pump blood out to the lungs and body. This cycle is called a heartbeat.
The normal adult heart rate is 60 to 100 beats per minute while at rest. Infants and children have a faster heart rate than adults.
Supraventricular Tachycardia
Supraventricular tachycardia (soo pruh ven TRIK yuh ler tack ih KAR dee uh), also called SVT, is a very fast heart rhythm that does not follow the regular pathway from the atria to the ventricles. It can cause a heart to beat at rates of 180 to 220 beats per minute in children and up to 300 beats per minute in infants. It can happen at any age and may be your child’s only heart problem. SVT can start and stop quickly. It may last for minutes or continue for hours. If it is not treated, the heart’s ability to pump normally is affected. SVT can occur at rest or be triggered by exercise. There are different types of SVT so your pediatric cardiologist will give more detail on which type of SVT your child has.
Common Signs and Symptoms
Infants are not able to tell you if the following signs or symptoms happen. They are not unique to SVT. They can occur with other illness.
- irritable
- poor feeding
- baby sweats a lot with feeding
- fast breathing (tachypnea)
- pale or generally ill appearing
Toddlers and older children may be able to tell you if they are having the following symptoms:
- heart pounds
- heart 'beeping' in chest
- feels a rapid or irregular heartbeat
- feeling pulses in their throat
Diagnostic Tests
If your child’s doctor thinks your child has SVT, you will be sent to a pediatric cardiologist who treats heart rhythm problems. They may recommend the following tests:
ECG/EKG (Electrocardiogram)
This test records the heart rhythm and can be done in a doctor’s office.
- The child’s shirt is removed.
- Small stickers are placed on the child’s chest.
- The stickers are connected by wires to an ECG machine.
- The ECG machine records the electrical activity in the heart.
- The stickers are removed from your child’s chest
You will get results as soon as the test is done. The test helps find abnormal electrical activity in the heart. The test does not hurt, but your child needs to be calm and rest during the test.
Holter Monitor
This test is an ECG that is recorded for 24 hours or more. The Holter is a monitor that your child goes home with. It records the heart rhythm during the day and while sleeping. This test is often used in children who may have a heart rhythm problem but are not able to tell you how they are feeling or what may be wrong.
Event Monitor
This is a special type of monitor. It can be worn for up to 30 days and allows your child to press a button to record the rhythm when they have symptoms. The recordings are sent to a monitoring service and then reported to the pediatric cardiologist for review.
Treatment
Your child’s pediatric cardiologist may recommend medicines or a procedure. Some of the choices are listed below.
Vagal Maneuvers
The vagus nerve is a nerve in the body that travels from the brain down through the chest and into the abdomen. The vagus nerve can slow down the heart rate. Older children may be able to slow their heart rate by trying one or more of the following:
- blowing through a straw
- doing a headstand
- bearing down or pretending to have a bowel movement
Medicines
Your child’s pediatric cardiologist may prescribe a medicine they take each day to treat SVT.
- Medicine does not cure SVT. It decreases the number of events and helps control symptoms by keeping the heart rate from beating too fast. This type of medicine is called a beta blocker.
- If the beta blocker does not work, another type of medicine may be used. These are called anti-arrhythmic medicines.
Ablation
This is an outpatient procedure done by a pediatric electrophysiologist (a heart doctor that specializes in abnormal rhythms). It is performed in the heart catheterization (KATH ett urr izz AY shun) lab. During the procedure, special equipment finds the electrical pathway in the heart that causes SVT. Ablation may be a choice if the medicine does not work or if your child still has frequent SVT symptoms. Your child will receive sedation or general anesthesia for the procedure.
Home Monitoring
For infants, you will be instructed to place your hand on your baby’s chest while they are calm and count their heart rate for one minute at least one time each day.
Children may be able to tell you if their heart is beating too fast.
- Not eating well
- Lethargic (tiredness)
- Irritable
- Excessive sweating
- Shortness of breath
- Dizziness
- Palpitations (feeling of the heart beating fast or fluttering)
If your child has SVT at home that is not relieved by vagal maneuvers or their medicine, get medical care. Go to your local emergency room or call 911.
In the emergency room, your child may get adenosine. This medicine goes through an IV, a tube that goes into the child’s vein and stops a fast heart rate so the heart can resume a normal rhythm. The medicine does this by slowing the speed of the electrical signal that is traveling through the heart.
Living with SVT
Most children with SVT live completely normal lives and have a normal life expectancy. However, it is important to routinely meet with your child’s pediatric cardiologist for continued SVT care.
- Keep important emergency phone numbers and doctor contact information in a place where you can easily access them.
- Write down all your questions as you think of them. Bring this list with you when you see the doctor.
HH-I-376 | Copyright 2020, Nationwide Children’s Hospital



