Scaphoid Fractures

The wrist is made up of eight bones. The wrist bone below the base of the thumb is known as the scaphoid bone. A fracture (break) of this bone can happen when a person falls onto the outstretched hand. This type of fracture does not happen very often in young children because this bone is mostly cartilage. It is seen more often in young adolescents. As more children participate in intense sports activities, this fracture is seen more often.
A person with a scaphoid fracture typically has pain at the wrist. Following a wrist injury, x-rays of the wrist will be taken. Right after a wrist injury, x-rays of the wrist may not show a scaphoid fracture. The provider may still place your child in a cast due to concern for an occult or ‘hidden’ fracture. X-rays will be taken at each follow-up visit; it is not unusual to discover a fracture where it was not clearly seen before.
Symptoms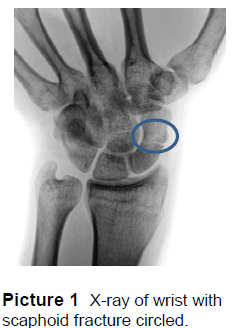
Your child may have swelling and bruising around the wrist. He or she may complain of pain when moving the wrist as well.
Diagnosis
X-rays of the wrist are taken to see if a fracture is present (Picture 1). This scaphoid fracture would be called a waist fracture based on its location in the middle third of the bone.
If the fracture is located in the bottom third of the bone it is known as a ‘proximal pole’ fracture.
On the top third of the bone, it is a ‘distal pole’ fracture. Where it is located will play a role in the treatment plan of the fracture.
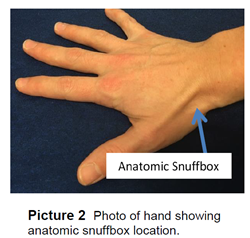
The provider will also do a physical exam to check for swelling, bruising, pain and range of motion. One area to check for pain is the “anatomic snuffbox,” shown in Picture 2. Pressing over this area puts pressure directly on the scaphoid bone. If there is pain at this area, the provider will presume there is a scaphoid fracture, even if it does not show on the x-ray.
Nonsurgical Treatment
A scaphoid fracture will need at least six weeks of immobilization in a cast, but often longer. We typically use a waterproof cast if no surgery is needed. We plan to see your child every four weeks to remove the cast, look at the skin, and get new x-rays. Depending on healing, he or she will be placed back in a cast or changed to a Velcro brace. Ninety percent of these fractures will heal with cast treatment, but it may take as long as three months, depending on fracture location.
Nonunion
A scaphoid fracture nonunion is when the
bone pieces fail to heal together. Typically
this occurs because of a missed or delayed
diagnosis.

A nonunion can also lead to avascular necrosis (AVN), when a lack of blood supply to a bone causes it to die. AVN can lead to early arthritis in the wrist. Blood flow to the scaphoid bone occurs via retrograde (‘backwards’) flow, meaning blood enters at the distal (top) portion of the bone and there is no direct blood supply to the proximal (bottom) portion of the bone. This retrograde blood supply is what can cause a fracture nonunion to go on to AVN (Picture 4).

Surgical Treatment
Some scaphoid fractures will need surgery to help them heal, especially those in the proximal pole or scaphoid nonunions. Surgical complications can include, but are not limited to:
- Bleeding
- Infection
- Harm to surrounding structures
- Nonunion (bone pieces do not
heal together) - Malunion (bones heal in wrong position)
- Hardware complications (screw breaks)
- Failure of fixation (fracture moves)
- Stiffness
- Wound healing problems
- Avascular necrosis (bone death)
- Need for further surgeries
This surgery is known as an open reduction and internal screw fixation. The surgeon will make an incision (‘cut’) at the wrist and insert a special compression screw to push the two pieces of bone together. Since there is no direct blood flow to the bottom piece of the scaphoid bone, pushing these pieces back together with the compression screw helps to direct blood flow to the bottom piece. This screw will stay in place for the person’s entire life. See Picture 5 for a before and after example of a scaphoid fracture that required surgery.
Sometimes a bone graft (piece of bone) is taken from the radius (forearm bone) to fill in the fracture of the scaphoid bone. The wrist is immobilized in a splint after surgery. Just as discussed before, these types of fractures need a splint known as a thumb spica splint.

The first follow-up is two weeks after surgery. The splint is removed and x-rays are taken. If the wound is healing well, the child will get a waterproof cast. Your child will continue to follow up in clinic every four weeks until sufficient healing is seen.
Some people benefit from the use of a bone stimulator. This is a device that can work through the cast to give off ultrasound waves that stimulate new bone to form.
The provider may order a CT scan to get a 3-D image of the bone. This shows how the healing is progressing. It helps to decide when we can stop casting and allow the child to return to normal activities with no restrictions.
When to Call the Clinic
Contact the orthopedic clinic if any of these things occurs:
- The splint or cast gets soiled, wet, or starts falling apart.
- Fingers are not pink and warm.
- Your child is crying more than usual or is in pain.
- Your child has a fever over 101oF after surgery.
Clinic Contact Information
- Clinic hours are Monday through Friday, 8:00 a.m. to 4:30 p.m.The phone number is (614) 722-5175. Ask for the nurse to discuss any symptoms.
- Evenings, weekends and holidays phone (614) 722-2000. Ask for the Orthopedic Resident on call to discuss any symptoms.
Be sure to contact the clinic if you cannot keep any follow-up appointments.
HH-I-439 6/18 | Copyright 2018, Nationwide Children’s Hospital



