Immune Thrombocytopenia (ITP)
![]()
Platelets are a kind of blood cell. These cells help the blood to clot after a person gets cut or bruised. The normal platelet count is between 150,000 and 450,000. A child with immune (ih MUNE) thrombocytopenia (THROM bow site oh PEE nia), or ITP, may have a platelet count of less than 1,000.
ITP happens when the body attacks and destroys its own platelets. This is called an autoimmune (aw toe ih MUNE) response.
ITP may have been started by a virus that your child had in the past. It is not contagious ("catching").
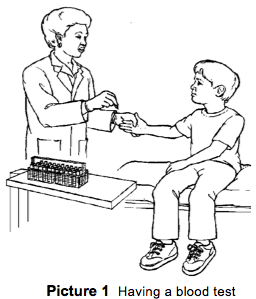
One of the tests your child will have is a blood test. A small amount of blood is taken to count your child's platelets (Picture 1).
Signs of Low Platelets
These are the common signs of low platelets. You may have seen some of these signs in your child:
- Bleeding that is hard to stop
- Nosebleeds
- Vomit that looks like coffee grounds
- Very easy bruising
- Bleeding gums
- Heavy menstrual bleeding
- Blood in the urine or stool
- Freckle-like, blue-purple spots - "tiny bruises" called petechiae (peh TEE kee ah)
Management of ITP
The goal of every treatment strategy for ITP is to end up with a platelet count that allows for minimal bleeding symptoms, rather than a “normal” platelet count. Patients with mild symptoms can be managed with observation alone, regardless of the platelet count.
Patients with heavier bleeding could discuss treatment options such as:
Steroids: Steroids help to keep platelets from being destroyed. They may be given by a pill, liquid or through an IV (intravenous tube). These steroids are not the same drugs that body builders take illegally.
Intravenous Immunoglobulin: This is a collection of antibodies taken from blood product. It can help keep platelets from being destroyed. Immune globulin is given by IV over 3 to 8 hours. More than one dose may be needed to improve the platelet count. For more information, read Helping Hand HH-II-17, IV Therapy.
Most patients can be managed with outpatient treatment. They may not need hospital admission. In most patients, ITP symptoms begin to improve within days to weeks and go away within several months. ITP that lasts more than 12 months is called chronic ITP. A child with chronic ITP may develop another autoimmune disease. Your child will have blood tests done to check for this.
What to Do at Home
- Bleeding is the major concern with ITP. Watch for signs of lowered platelet counts such as worsening bruising and petechiae, or heavier bleeding.
- Do not give medicine that contains aspirin or ibuprofen(Advil®, Motrin®, PediaCare Fever®, etc.) to your child. It can increase the chance of bleeding. Give acetaminophen (such as Tylenol®) instead.
- Use a soft toothbrush and continue regular, gentle brushing of your child’s teeth. Eating soft foods may help your child prevent mouth or gum bleeding.
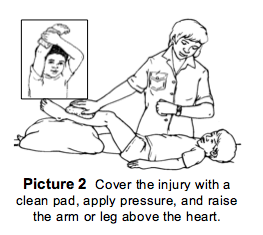
- If your child gets cut, put a clean gauze pad or cloth over the cut. Then apply pressure with your fingers for at least 5 minutes, or until the bleeding stops. If the cut is on the arm or leg, raise it above the heart (Picture 2). If you cannot stop the bleeding, take your child to the nearest emergency room for treatment. Be sure to tell the nurse and doctor in the emergency room that your child has ITP.
- Your child should not play contact sports or other activities with a high risk for falls. Encourage your child to remain active in other exercise activities.
- When your child rides a bike, he should wear a bike helmet and kneepads.
- Choose toys that do not have sharp edges.
- Ask your child's doctor when he may return to school, and if he may attend gym class or play non-contact sports.
When to Call the Doctor
Call your child's doctor if the child has any of the following:
- Increased bruising or petechiae
- Active bleeding
- Is hard to wake up
- Is not acting right
Follow-Up Appointments
Your child will have regular appointments with the doctor to check the platelet count. Be sure to keep these appointments.
If you have any questions or concerns, call the Nationwide Children’s Hospital ITP nurse clinicians at (614) 722-8915, or the Hematology Clinic at 614-722-3250, Monday through Friday, 8:00 am to 4:30 pm.
After hours, call the Nationwide Children’s Hospital operator at (614) 722-2000. The operator will contact the hematologist "on call." He or she will return your phone call.
HH-I-136 Revised 3/17 Copyright 1990 Nationwide Children’s Hospital

