MRSA Infection in the Community (Methicillin Resistant Staphylococcus Aureus)

Staphylococcus aureus (staf ill o COCK us ARE ee us), often simply called "staph," are common bacteria (germs). All of us have germs on our skin and in our noses. Some of these germs can cause infections if they get into breaks in the skin. In the United States, staph germs are some of the most common causes of skin infections.
Most staph infections are minor. These can be treated without antibiotic medicines. At other times staph germs can get into a wound and cause infection. This is more serious and needs to be treated with antibiotics.
In the past, serious staph infections were treated with a type of antibiotic related to penicillin. Some staph infections can still be treated with antibiotics in the penicillin family. Others have become resistant over time. These need antibiotics that are not penicillins.
- The germs that can still be treated with penicillin-like drugs are called Methicillin-Susceptible Staphylococcus Aureus, or MSSA.
- Germs that are now resistant to penicillin-like drugs are called Methicillin-Resistant Staphylococcus Aureus, or MRSA. MRSA is described as a multi-drug-resistant germ.
There are two main types of MRSA. Their names come from where you are exposed to the staph germ. One is called Community-Associated MRSA Infection (CA-MRSA). The other is called Healthcare-Associated MRSA (HA-MRSA). It is related to health care facilities, such as hospitals and nursing homes. This Helping Hand gives information on CA-MRSA.
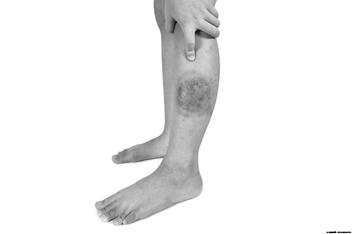
People can have MSSA and CA-MRSA germs in their bodies and not get sick. Infection occurs when the germs cause disease. Often, the first sign of disease is an infected abscess (boil) or red, raised areas, often mistaken for “spider bites”. If they are not treated, staph germs can cause bone infections, pneumonias or life-threatening bloodstream infections.
Risk Factors for MSSA and CA-MRSA
Staph infection is spread by direct contact or by touching contaminated things, not through the air.
Some risk factors for infection are:
- Sharing personal items like towels, sports gear, toothbrushes, combs, and razors
- Skin damage (breaks in the skin) caused by minor trauma like a cut, burn, or insect bite
- Skin damage caused by a medical condition, like eczema, that has weakened the skin
- Weakened immune system
More Risk Factors Specific to CA-MRSA Include:
- Recent, frequent antibiotic use
- Close contact with others (such as in gym class, contact sports, or a locker room) who may have CA-MRSA germs on their skin
- Living or spending a lot of time in crowded areas, like daycare centers
- Getting tattoos and piercings by people who are not licensed, or at a place that is not clean
Treatment of MSSA and CA-MRSA
Many staph skin infections are treated just by draining the boil. The doctor will do a test to decide what type of germ is causing your child’s infection and which antibiotic will work best. MSSA infections are treated with antibiotics related to penicillin. MRSA infections are harder to treat. They require antibiotics that are not in the penicillin family. These drugs may have more side effects than penicillins.
It is very important to take all the medicine as ordered.
- If an ointment is prescribed for treating an infection, apply it to all the skin sores, even the tiny ones.
- Sometimes the doctor may order antibacterial ointment to be placed in the child’s nose, or a special soap for bathing. This is done when there is a concern that the child is “carrying” the staph germs in the nose, rectal area or on the skin even if those areas look normal.
- If an incision was made and the area was packed with a gauze dressing, your doctor may want your child to come back to have the wound checked and repacked.
- Your doctor will tell you if your child can participate in school activities, such as gym.
Other Family Members
Family members and pets may be at risk for getting the MSSA and CA-MRSA staph infection or carrying the germs. If family members have boils or infected sores, they should call their doctor for advice.
If you see signs of skin infection on your pets, call your veterinarian.
Preventing the Spread of Infection
- Wash your hands often for 15 to 20 seconds (Picture 1). Use a hand sanitizer or antibacterial soap and water, especially if you have touched infected skin or bandages.

- Do not share personal items. Teach your child not to share towels, sports gear, toothbrushes, razors, combs and clothing.
- Cover wounds. Keep cuts, scrapes and sores clean. Cover them with a clean bandage until healed. Place soiled bandages in a separate trash
bag and close tightly. - Do not touch other people’s wounds or items that have touched their wounds. Teach your child not to touch or pick at
a wound. - Wash clothes and bedding on the hottest settings. Use bleach whenever possible.
- Shower after athletic activities, especially contact sports.
- Check your child’s skin during bathing for any signs of new boils (Picture 2).
- Wear rubber gloves to scrub the bathtub after each use. Use a bleach solution or bathroom cleanser that contains bleach.
- Children with boils or draining wounds should not participate in contact sports or activities with close contact to others until the infection is completely healed.
- Tell the school nurse, homeroom teacher, gym teacher and others who will have
close contact that your child has CA-MRSA.
When to Call the Doctor
Call your child’s doctor if:
- Your child gets worse (more swollen, more painful, redder; more ill-appearing)
- Your child develops a fever, has hard time breathing or has other signs of getting worse (such as vomiting, diarrhea, always sleeping)
- Your child or another family member develops new skin sores or boils
- Your child will not or cannot take the medicine that the doctor prescribed
About Your Child’s Medical Record
What a Diagnosis of MRSA in Your Child’s Medical Record Means
Until the MRSA diagnosis is removed from your child’s record, every time your child is admitted for an inpatient stay he or she will be placed on Contact Precautions. Because MRSA germs are spread when someone touches (contacts) your child or items in the room that may have been touched by your child, you will see your child’s caregivers putting on and wearing a protective gown and gloves before entering the child’s room. Your child will have to stay in his or her room and will not be able to walk the hospital halls until discharge.
Removing the Diagnosis of MRSA from Your Child’s Record
After your child is diagnosed with MRSA, the diagnosis will stay in his or her medical record until these things are done:
- Your child needs to be out of the hospital and off antimicrobial therapy and invasive devices for six months. Then:
- A Culture MRSA Screen (MRSAC) test to check for active MRSA needs to be ordered by your child’s pediatrician.
- This test can be done at your child’s pediatrician’s office during a routine visit, at a Nationwide Children’s Hospital’s Urgent Care, or scheduled by the parents at a Nationwide Children’s Hospital’s test center they choose.
- If the original diagnosis was from a respiratory infection, there need to be three cultures taken from the nose. All three need to test negative for Multidrug-Resistant Organisms (MDROs). These cultures need to be taken at least 72 hours apart with no hospitalization, off antimicrobial therapy and no invasive devices in between.
- If the original diagnosis was from a non-respiratory site (wound, drainage, blood urine, etc.), there need to be three cultures from the nose and three from the rectum that test negative for MDROs. These cultures need to be taken at least 72 hours apart with no hospitalization, off antimicrobial therapy and no invasive devices in between.
If you have any questions, be sure to ask your doctor or nurse.
HH-I-244 11/04, Revised 10/17 Copyright 2004, Nationwide Children’s Hospital