Osteosarcoma

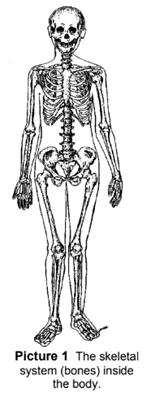
Osteosarcoma (OS tee oh sar KOMA) is a cancer of the bone. It starts in immature bone cells that normally form new bone tissue. The tumor is usually located near the ends of the long bones in the legs.The next most common site is the upper arm bone near the shoulder. It can also occur in other bones such as ribs and pelvic bones (Picture 1).
Osteosarcoma destroys tissue close to the tumor and weakens the bone. This type of tumor usually occurs in teens and young adults, but can occasionally occur in younger children.
The cause of osteosarcoma is not known. Most of them develop in people who have no other diseases and no family history of bone cancer. In a very small number of families, siblings develop osteosarcoma.
Signs and Symptoms
Often the earliest sign of osteosarcoma is pain. Swelling, warmth and redness may occur in the area over the affected bone. A bone that breaks without injury or with minimal injury or trauma may occur.
Diagnosis
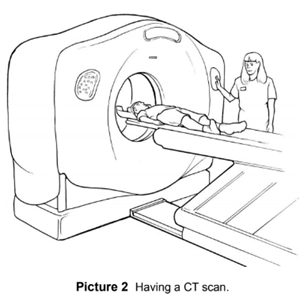
An X-ray of the bone may suggest osteosarcoma, but a biopsy (a sample of the tissue of the affected bone) is needed to make a definite diagnosis. An MRI test (Magnetic Resonance Imaging) will be done to decide the extent of the disease. A surgeon will do the biopsy in the Operating Room. A pathologist will then look at the tissue under a microscope.
Because osteosarcoma can spread to other parts of the body (metastasis), a careful look for this spread is made before any further surgery or treatment is done. A chest X-ray or chest computed tomography (CT scan) (Picture 2) will be done to check for spread to the lungs.
A bone scan is done to look for tumors in any other bones.
Doctors use the following terms to describe osteosarcoma and develop treatment plans:
- Localized: The tumor is limited to the bone where it started and the tissue around the tumor; it has not spread to other parts of the body.
- Metastatic: The tumor has spread from where it began to other parts of the body. The most common sites of spread are the lungs or other bones.
- Recurrent: The tumor has come back after treatment. It can recur in the same place that it started, or in another part of the body. The lungs and other bones are the most common sites of recurrent tumors.
- Initial response to therapy: One of the best ways to predict treatment success is how the child responds to the start of therapy. Patients whose tumor cells are nearly all gone after the first 10 weeks of chemotherapy have a better outlook than those whose tumor cells do not respond as well to treatment. If the likely response to treatment can be determined at the time of diagnosis, treatment can be more targeted. This could improve the outlook for patients with less responsive tumor types.
Treatment
Most of the time, chemotherapy is the first treatment for osteosarcoma. The type, amount and how often the chemotherapy is done is decided by the oncologist (cancer doctor). The goal of chemotherapy is to reduce the size of the tumor.
The next treatment step is surgery. The type of surgery depends on the tumor. An MRI test is repeated before surgery to help the surgeons plan their treatment. A piece of the bone may be removed or a large part of bone may be removed and replaced with bone taken from another part of the body (such as the hip) or with a metal rod.
If possible, a custom implant replaces the bone where the tumor was located and is adjusted as the child grows. This is called "limb sparing." Another possible surgery is amputation (removing) of the affected leg or arm. An amputation of the affected limb may be done when limb sparing is not possible because of the size and location of the tumor. Your child’s surgeon will discuss surgery options with you.
Follow-Up Care
- Your child will have follow-up appointments with an oncologist. This doctor will monitor your child's progress and watch for side effects of the treatment.
- X-rays and CT scans are done at times to check for spread of the disease.
If you have any questions or concerns, be sure to talk with your doctor or nurse.
HH-I-130 6/90, Revised 5/17 Copyright 1990, Nationwide Children’s Hospital

