Intracranial Hypertension (Pseudotumor Cerebri)
Idiopathic intracranial hypertension, sometimes called pseudotumor cerebri, is a condition in which the cerebro-spinal fluid is not able to drain normally.
What Is Idiopathic Intracranial Hypertension?
Idiopathic intracranial hypertension, sometimes called pseudotumor cerebri, is a condition in which the cerebro-spinal fluid (the fluid inside the skull) is not able to drain normally. When no underlying cause is detected for the elevated pressure, the condition is said to be “idiopathic.” The term “pseudotumor” is sometimes used because the extra fluid mimics the effects of a brain tumor by pushing against the brain.
Common symptoms of intracranial hypertension are headache and vision problems. The most common cause of this condition in children and adults is obesity. However, many patients have the condition even if they are not overweight.
What Are the Risk Factors for Intracranial Hypertension?
So far, we know of three factors that increase the risk of having intracranial hypertension:
- Obesity
- Being female
- Being a teen
Some medicines increase the risk of developing intracranial hypertension. These include medicines used to treat acne, steroids, growth hormone, antibiotics, thyroid replacement medicines and some chemotherapy drugs. Other disorders that can lead to intracranial hypertension include kidney disease, head injuries, lupus, severe sinus infections, ear infections, measles, blood-clotting disorders, anemia and malnutrition. When medicines or other conditions are the cause, it is called “secondary intracranial hypertension.”
Can Children Develop Intracranial Hypertension?
Yes.
- Children (both boys and girls) who have not reached puberty
- Teenagers who have reached puberty and have the risk factors listed above
What Does the Optic Nerve Look Like?
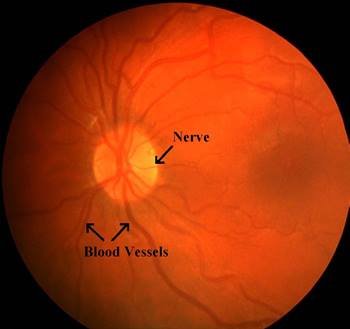
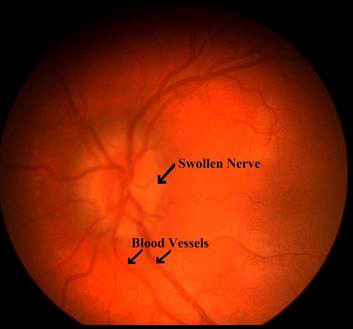
Left: This is how the eye normally looks. Right: Eye of a patient with intracranial hypertension.
What Are the Symptoms of Intracranial Hypertension?
Symptoms can include any of the following:
- Headaches each day with pulsing or throbbing above the eyes, or at the back of the head and neck. These headaches are often worse when lying down or in the morning.
- Any movement that increases pressure in the abdomen (like coughing, bearing down, or bending over) that makes the headache worse
- A whooshing or ringing sound in one or both ears
- Double vision (due to pressure on the nerves controlling eye movement)
- Brief changes in vision, like short-term dimming or blacking out
- Peripheral vision (vision out to the sides) fades or gets blurry or black
- Dizziness, nausea and vomiting
What Causes Intracranial Hypertension?
The exact cause is not known. However, we do know if the body makes more cerebrospinal fluid than the amount absorbed, it causes the pressure inside the skull to increase.
How Do We Diagnose Intracranial Hypertension?
For symptoms of intracranial hypertension, an ophthalmologist (eye doctor) usually looks for swelling of the optic nerve in the back of the eye, and for signs of vision loss. Some diseases can appear the same as intracranial hypertension. Tests like a CT or MRI scan help to rule out these diseases. If the imaging does not show a cause, the next test is a lumbar puncture (spinal tap). This test measures the pressure inside the skull, and removes some of the cerebrospinal fluid. Intracranial hypertension is diagnosed if the symptoms listed above are present and there is elevated pressure inside the skull.
Why Do We Treat Intracranial Hypertension?
The increased pressure causes headaches and injury to the optic nerves. If the pressure is not corrected, the nerve injury can cause blindness.
How Is Intracranial Hypertension Treated?
The ophthalmologist will closely monitor your child’s vision and the nerve swelling. Medicines to lower the pressure and bring down the nerve swelling are the most common treatment. There are three groups of medicines used alone or together.
While less common, sometimes surgery is done to help lower the pressure. This can include placing small cuts in the covering of the nerve (optic nerve fenestration), or a tube (shunt) to slowly remove some of the cerebrospinal fluid (in the spinal canal, or inside the skull).
At Nationwide Children’s Hospital, we have a special clinic for patients with intracranial hypertension. Typical office visits include exams by an ophthalmologist and a neurologist. Sometimes patients in our clinic are also seen by specialists from Neurosurgery, Hematology, Psychology and Healthy Weight and Nutrition.
Are There Treatments Besides Medicine and Surgery That Can Help?
The most important thing anyone can do to improve this condition is to maintain a healthy weight, or lose weight if obese. If your child needs to lose weight, ask your doctor about local resources and clinics that can help.
What Is the Outcome of Intracranial Hypertension?
If treated, the outcome is good. If not treated, permanent blindness can occur. Unfortunately, up to one in 10 people with intracranial hypertension have some vision loss. Treatment typically lasts six to 12 months. With treatment, in most cases, this condition goes away. However, increased pressure can return months or even years later. You can reduce this risk by helping your child maintain a healthy weight. It is important to have regular eye exams to check for vision loss even after the intracranial hypertension gets better.
Physician Referral Information
The Intracranial Hypertension Clinic accepts referrals from primary care physicians and pediatric specialists from the United States and internationally. To make a referral, there are three options:
-
Fax a referral request to (614) 722-4000
-
Make a referral and schedule by phone at (614) 722-6200 or 1-877-722-6220



